The basics every survivor should know about breast cancer–related lymphedema
Lymphedema is one of the most misunderstood and under-discussed side effects of breast cancer treatment. I recently shared a blog post about my own personal lymphedema experience. Now I want to provide you with all the basics every survivor should know to help reduce risk or manage lymphedema.
This post is meant to give you a clear, foundational understanding of what lymphedema is, why it happens, how to reduce your risk, and how it’s managed long term, not to cause fear, but because knowledge is power. And too many survivors are never given the critical education they need.
What is lymphedema?
To understand lymphedema, it helps to first understand the lymphatic system.The lymphatic system plays two crucial roles: maintaining fluid equilibrium and functioning as a part of the immune system.
It’s a network of lymph vessels and lymph nodes that:
- Collect excess fluid, proteins, and waste from tissues
- Filter that fluid through lymph nodes
- Return it back into the bloodstream
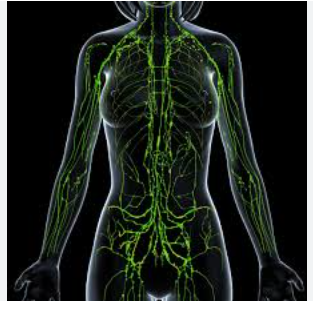
The lymph system is responsible for pumping lymph fluid throughout your body, but it does not have its own pump. Instead, it relies on:
- Muscle contractions
- Joint movement
This is why movement is so important for lymphatic health.
Lymphedema occurs when the lymphatic system’s ability to transport fluid is reduced and the amount of lymphatic fluid present becomes too much for the lymph system to handle. Over time, lymphatic fluid begins to accumulate in tissues and this can lead to swelling, heaviness, tightness, skin changes, and tissue thickening.
Lymphedema isn’t caused by “doing something wrong.” It’s caused by reduced lymphatic capacity coupled with a lymphatic load that is too high.
Increased inflammation in the body can lead to a lymphatic load that is too high. Systemic inflammation places additional demand on the lymphatic system.
Things like:
- Infection
- Allergic reactions
- Certain medications
- High stress
- Poor sleep
can all lower the threshold at which lymphedema symptoms appear. Managing inflammation matters, not just locally, but systemically.
What causes breast cancer–related lymphedema?
Breast cancer–related lymphedema most commonly develops as a result of:
- Lymph node removal via sentinel lymph node biopsy or axillary node dissection
- Radiation therapy, which can cause fibrosis and scarring of lymphatic vessels
These treatments are often life-saving, but they permanently change the lymphatic system. These changes lead to reduced lymphatic capacity, which can result in lymphedema.
Anyone who has had lymph node removal of any type, or radiation to the lymph nodes is at risk of developing lymphedema. Unfortunately, we are currently unable to predict exactly who will go on to develop lymphedema, but there are things that we can do to help reduce the risk.

Reducing your risk of developing lymphedema
While lymphedema isn’t always preventable, there are ways to reduce risk and support lymphatic health:
1. Address cording, fibrosis, and scar tissue early
Radiation fibrosis, surgical scarring, and axillary web syndrome (cording) can restrict lymphatic flow. Early, targeted therapy is so important.
2. Exercise (the right way)
As discussed above, movement helps the lymphatic system function via muscle pumping and joint movement. Progressive, lymphatic-friendly movement and resistance training supports lymph flow and lymph system resilience.
3. Maintain a healthy BMI
Higher BMI is associated with increased lymphedema risk, likely due to increased inflammatory load and mechanical demand on the lymphatic system.
4. Recognize early signs
Your lymphatic system often gives subtle signals before visible swelling appears:
- Tightness
- Heaviness
- Achiness
- Intermittent puffiness
- Changes that come and go
These signs are your body’s way of telling you that your lymph system is stressed. Pay attention to these.
Work within the current capacity of your lymphatic system
This is one of the most important concepts to understand.
Many breast cancer treatments result in a lowered capacity of the lymphatic system. The good news is that the capacity of your system CAN be improved. But it is so important to always function within the CURRENT capabilities of your lymphatic system to prevent overload and stress.
Overloading the lymphatic system, through repetitive strain, inflammation, infection, or “ doing too much too soon” can push it beyond what it can handle at that time, leading to lymphedema.
Learning to work with your lymphatic system instead of against it is key to risk reduction and prevention of progression of lymphedema.

Stages of lymphedema: reversible vs. chronic
Lymphedema is classified into 4 stages:
- Stage 0: No visible swelling, but the lymphatic system is compromised. Symptoms may include heaviness or tightness.
- Stage 1: Mild, visible swelling that may fluctuate and often improves with elevation or compression.
- Stage 2: Persistent swelling with tissue changes; does not fully resolve with elevation.
- Stage 3: Advanced swelling with skin changes and fibrosis.
Early stages are far more manageable, and often reversible. Later stages (stage 3 and 4) are more permanent, and more difficult to manage.
Why early recognition and treatment matter
Catching lymphedema in the early stages:
- Means it is more likely to be reversible
- Makes it easier to manage
- Reduces the risk of progression
- Preserves tissue health
- Improves long-term outcomes
This is why awareness and early intervention are so critical. And too often, we are provided with little to no information about the early signs to watch for.
Management of lymphedema
Lymphedema is a chronic condition, but it can be managed. The gold standard approach is Complete Decongestive Therapy (CDT), which includes:’
1. Manual Lymphatic Drainage (MLD)
Gentle, specific techniques to encourage lymphatic flow.
You can check out my MLD Handout to learn more about this technique and how to perform it.
2. Compression
Sleeves, gloves, bras, or bandaging to support fluid movement and prevent accumulation.
3. Exercise and movement
Movement improves lymph flow due to muscle contraction and joint movement.
4. Skin care
Reducing infection risk and maintaining tissue health.

Exercise does NOT cause lymphedema
This is one of the most persistent myths. Exercise does not cause lymphedema, in fact, it helps manage it. However, it must be:
- Progressive
- Symptom-guided
- Appropriate for your treatment history
- Respectful of healing tissues
This is the premise that all Pink Badger Exercise Programs are built on. It’s important to exercise in a way that is appropriate for your particular stage of treatment or recovery.

How to find a lymphedema therapist
If you are at risk of lymphedema or if you develop any signs of lymphedema, I highly recommend seeking intervention ASAP. Medical providers don’t always suggest therapy, but you can always ask for a referral. I strongly recommend working with a specialized physical or occupational therapist, rather than a general orthopedic provider.
Look for credentials such as:
- CLT (Certified Lymphedema Therapist)
- CLT-LANA
- Board Certified Oncology Clinical Specialist
- PORi Certified Breast Cancer Rehabilitation Therapist
- PORi Certified Breast Cancer Rehabilitation Specialist
These designations indicate advanced training specific to oncology and lymphatic care.
Here are a few directories to help you find a specialized provider in your area:
- Lymphatic Education & Research Network
- Oncology PT Directory
- Norton School CLT Directory
- CLT-LANA Directory
- PORi Therapist Finder (You’ll find me here, based in Homer, AK!)
Word-of-mouth recommendations within survivor communities can also be invaluable.
Final thoughts
Lymphedema is common. It is often overlooked. And it is not hopeless or a personal failure.
With education, awareness, and early care, lymphedema can be managed, and quality of life can be protected.
You deserve clear information, real guidance, and support that understands what your body has been through.